It was a bit more than two decades ago that “shock waves” were introduced into veterinary medicine as a treatment for orthopedic injuries (mostly). Using a simple non-invasive probe, horses could be treated for a variety of injuries and conditions causing lameness, including, but not necessarily limited to, arthritis, back pain, tendon injuries, skin wounds, and navicular syndrome (and, presumably, indigestion and bad hair coats, too). It was simple! It was amazing! It was wonderful! It sounded almost too good to be true!
It was a bit more than two decades ago that “shock waves” were introduced into veterinary medicine as a treatment for orthopedic injuries (mostly). Using a simple non-invasive probe, horses could be treated for a variety of injuries and conditions causing lameness, including, but not necessarily limited to, arthritis, back pain, tendon injuries, skin wounds, and navicular syndrome (and, presumably, indigestion and bad hair coats, too). It was simple! It was amazing! It was wonderful! It sounded almost too good to be true!
It’s looking like it was (too good to be true).
ETYMOLOGICAL ASIDE (I can’t help myself). The Oxford English Dictionary finds the phrase “too good to be true,” all the way back in 1580. More recently, people have said, “If it sounds too good to be true, it probably is.” Finding out where the rest of the phrase comes seems to be more problematic, but this sort of challenge is the sort of thing on which etymologists build careers. Anyway, you know what I mean, and, if you don’t, you should.
 The late 1990’s and the early 2000’s was just chock full of wonderful glowing testimonials about using shockwave for just about everything. And you should have seen the floor space rented at veterinary conventions. The units sent pulsed and energetic “shockwave” into the tissues that…. well, no one was really exactly sure what it did, but whatever it was, it was sure supposed to be good. Veterinarians rushed to buy the units – horse owners rushed (and paid for) to have them applied. The horses, of course, didn’t say anything – come to think of it, that’s one of the beauties of horses, actually. Thus, with very little good evidence that the therapy did anything, yet another “promising” intervention was introduced to the horse world (and, it’s still used, to be sure).
The late 1990’s and the early 2000’s was just chock full of wonderful glowing testimonials about using shockwave for just about everything. And you should have seen the floor space rented at veterinary conventions. The units sent pulsed and energetic “shockwave” into the tissues that…. well, no one was really exactly sure what it did, but whatever it was, it was sure supposed to be good. Veterinarians rushed to buy the units – horse owners rushed (and paid for) to have them applied. The horses, of course, didn’t say anything – come to think of it, that’s one of the beauties of horses, actually. Thus, with very little good evidence that the therapy did anything, yet another “promising” intervention was introduced to the horse world (and, it’s still used, to be sure).
One of the problems with many treatments and devices in the horse world is that they get thrown out there for everyone to try well in advance of the evidence that they actually do anything. This isn’t just a problem with shockwave, by the way, it’s a problem with stem cells, and magnets, and lasers, and any number of “promising” therapies that I’ve seen come and go over the past (gasp) three decades or so. My three decades is something of a drop in the bucket for some therapies, for example, I ran across an old book at the UCLA medical school library from the late 1700’s touting the miracles of magnets. But when a therapy is new, when it’s different, when it’s “cutting edge,” when it can be tried on conditions for which there is no quick, satisfactory, or sure cure, and when there is no strict premarket testing required, it hits the market, and away people go!
After a time, however, those stodgy old scientists start to look into treatments and devices (that’s one of the things that scientists do), and, after a time, scientific evidence starts to catch up. This can be either a good or bad things in terms for proof of effectiveness for the proposed therapy; unfortunately, when it’s bad news, the evidence shows up long after people have invested lots of money in them. And it turns out that when it comes to shockwave, the past decade or so has provided some very good studies that mostly show that the units are not only not what they’re cracked up to be, but that they’re really not very much at all. People still use them of course – science is often not nearly as persuasive as earnest testimonials. Anyway, when it comes to scientific evidence and “shock wave,” here goes (and you can read for yourself, on a couple of them).
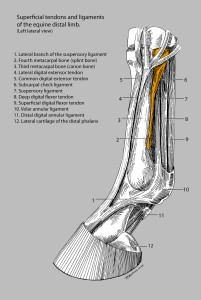
In June, 2011, research in the journal Veterinary Surgery concluded that “Shockwave” Therapy (Extracorporeal Shock Wave Therapy, or ESWT) does nothing for experimentally induced injuries to the “check ligament” of the horse’s forelimb. The significant clinical results? Zip. Nada. Bupkis.
CLICK HERE to read the abstract in Veterinary Surgery.
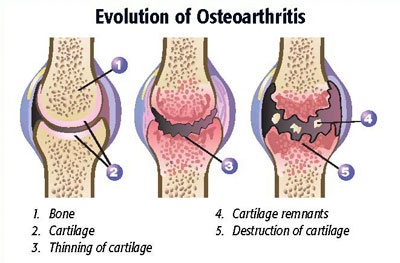
In June, 2011, researchers at Colorado State University “shocked” joints with experimentally-induced arthritis. They found that shockwave had no effect on the bone under the cartilage (as one might hope), even though they found an increase in some substances in the blood that may be associated with bone activity (it’s called remodeling). I guess that can be interpreted as good news of some sort, but the problem is that no one really knows what an increase in substances in the blood means in relationship to treating arthritis. Otherwise stated, they found something, but who knows what it means?
CLICK HERE to read the abstract of the study from the American Journal of Veterinary Research.
In addition to these studies, there has been a veritable parade of negative or insignificant studies over the past few years that have found no significant effects on wound healing, possible harmful effects on normal tendons (CLICK HERE and HERE), no effects on experimentally induced check ligament injuries (CLICK HERE), no effects on wound healing (CLICK HERE), no effects on collateral ligament injuries of the joint of the foot (CLICK HERE), no effect on X-rays or “bone scans” in horses with pain in the back of the foot (CLICK HERE), no changes on ultrasound in experimental injuries to the superficial digital flexor tendon (CLICK HERE), and, at best, a short term analgesic (pain-relieving) effect in the legs (CLICK HERE and HERE). More recently, in one uncontrolled study (that is, not as good of a study as it could have been), examining twelve horses with back pain, shockwave was said to have an analgesic effect. (CLICK HERE),
A NOTE ABOUT SHORT-TERM ANALGESIC EFFECTS: If shockwave causes short-term analgesia – read: numbness – that’s not necessarily a good thing. You don’t want an athletic horse feeling numb anywhere, because that increases the risk for injury to horse and rider. Which is why most authorities ban the use of shockwave before competitions: just in case.
Now here’s the thing. In fact, you can take this comment to the bank. IF A THERAPY IS REALLY EFFECTIVE, IT DOESN’T TAKE LONG FOR EVERYONE TO BE ABLE TO SHOW IT’S EFFECTIVE. That’s the way things work. For example, in 1942, doctors gave a very sick lady named Anne Miller a small dose of penicillin, and the next morning, to everyone’s amazement, she was up and eating. Within no time, the production and use of antibiotics exploded (CLICK HERE to read Anne Miller’s obituary in the New York Times – she died in 1999, at the age of 90).
That’s the way things go when medications or therapies are truly effective – everyone figures it out, figures out the best way to use them, and medicine moves forward. If something works, future studies generate increasingly clear and accurate observations over time. On the other hand, ineffective therapies give random results. Over time, when therapies don’t work, negative results accumulate. Of course, it’s usually possible to find positive studies, too, which generally leads to reference duels. Suffice it to say that after more than two decades, the positive evidence for shockwave has not accumulated and people are still trying to figure out how, and more importantly, IF, it does anything meaningful in terms of healing.
I say, ‘Trying to figure out,” of course, because, in fact, nobody is really trying that hard, it seems. The therapy is out there, it gives folks something to do, it doesn’t cause overt harm, and people will pay for it. For me, however, that’s not good enough.
I’m rarely the first one on board with a new technology, simply because I’ve seen so many of them come and go. I’d rather not ask my clients to fork over lots of money to pay for something that I can’t say how if or even if it works. And, based on the latest information, I’m sure not about to buy a shockwave machine now (a colleague of mine says that it’s best used as an anchor for his bass boat). Bottom line? In my opinion (and I promise you, you’ll find other opinions, particularly if it comes from someone who owns or sells a shockwave machine), I don’t really think the therapy merits much attention. And, come to think of it, I haven’t seem quite as much space devoted to the machines on veterinary convention floors lately, either.
THE BOTTOM LINE? The benefit from shockwave, if any, seems quite modest, at best. It might cause some short-term analgesia, but the cost is a sure thing. “You pays your money and you takes your chances,” is not much of a motivator to use any therapy, in my opinion.