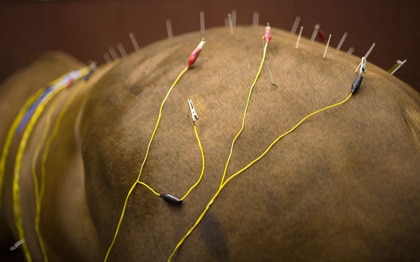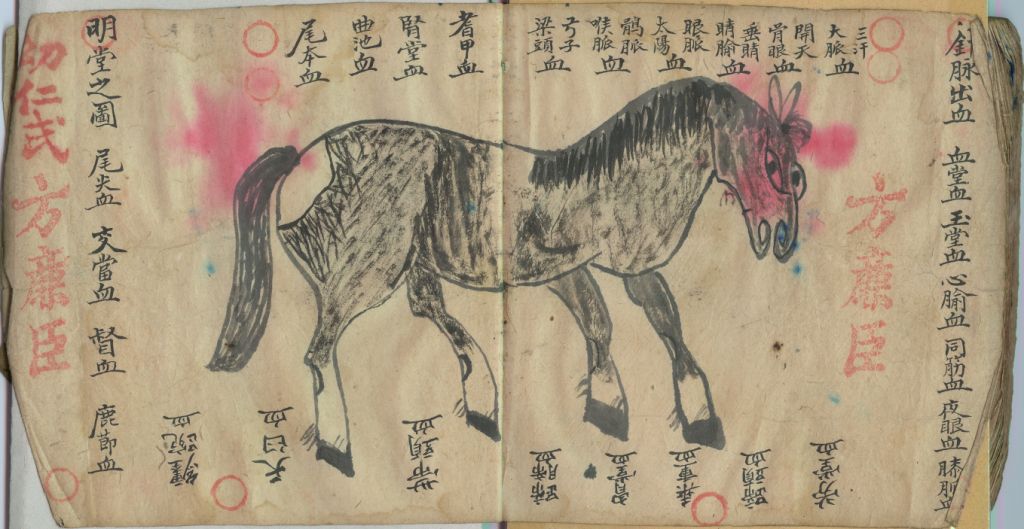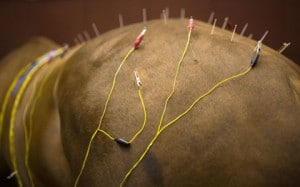
Equine Acupuncture
Dr. Ramey sticks a pin in the argument for acupuncture
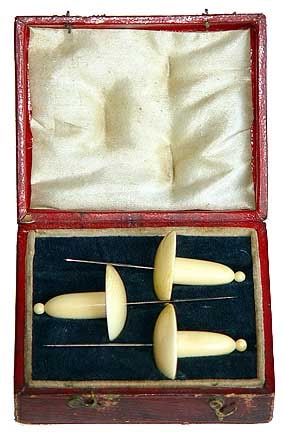
Acupuncture is big business these days, with people queuing to have sharp needles stuck in their bodies in the hope of achieving some sort of therapeutic effect. The practice has been presented to curious westerners as the quintessential ‘Chinese medicine’, used for millennia for the effective treatment of a wide variety of ailments. Unfortunately, almost everything that has been presented to a gullible public by enthusiastic proponents and naive journalists has been wrong. From a historical standpoint, 20th century scholars have imagined a trial and error system of development whereby knowledge was collectively accumulated into a medical ‘system,’ and have thereby asserted that acupuncture has withstood the test of time. One view has been that, over time, crude stone lancets were replaced with fine metal needles, and acupuncture points and channels were codified, leading to a new age of medical sophistication. However, there is now considerable doubt about the existence of a trial and error system, as well as the assumption that ‘needling,’ as described in historical Chinese medical texts, is today’s acupuncture. Indeed, despite antecedent ideas and practices, modern acupuncture, with such strange aspects as electroacupuncture, may never have existed in traditional China in anything like the form that it is practiced today. In addition, the ‘test of time’ is certainly an inadequate standard; witness the persistence of astrology.
Nor is acupuncture typical of the historical practice of Chinese medicine. Indeed acupuncture, and much of what is presented as ‘alternative’ Chinese medicine, is only a minimal vestige of ideas and practices. The adaptation of Chinese medicine, promoted in China as zhongyi since the mid-1970s is, in fact, not an accurate reflection of the tradition of Chinese medicine, measured from ancient times to the present.
But historical misrepresentations aside, what of the current practice of acupuncture? Over the past three decades there have been literally thousands of studies on acupuncture published in dozens of medical journals for myriad conditions. Such studies vary greatly in quality, from well-designed clinical trials to uncontrolled testimonials, from individual case reports to laboratory investigations on animals. The only consistent feature of such studies has been the randomness of the results obtained. In 1999 a study published in the American Journal of Acupuncture stated that “thirty years of active acupuncture research … failed to unequivocally demonstrate its clinical efficacy,” a situation that remains unchanged today.
But what of acupuncture’s effects? It is inarguable that individual studies may show positive results, whether it be in studies of the treatment of individual conditions (eg back pain, headache) or in studies designed to search for mechanisms of action (eg functional MRI studies looking for brain activity after acupuncture). But even when effects can be demonstrated, it’s not at all clear that these effects have any meaning for clinical patients. Regardless, the proponents of acupuncture still have to deal with many quandaries.
First, neither acupuncture points nor ‘meridians’ have ever been shown to exist. That’s right – the most fundamental structures of the practice cannot be reliably demonstrated. Research on the nature of acupuncture points and meridians is often difficult to evaluate because of the diverse nature of the claims made, incomplete data provided in published studies and the variety of parameters involved in the assessment of these claims. Obvious contradictions exist between current acupuncture practice and the historical record, as well as on the ‘correct’ number of points and meridians reported by current practitioners of acupuncture. From a pragmatic standpoint, one might surmise that if such structures did exist and could be reliably demonstrated, they would revolutionize the study of anatomy and physiology; no such revolutions have yet been forthcoming. Whatever the clinical efficacy of needling, there is, as yet, no compelling evidence to show that acupuncture points or meridians exist as discrete entities. Indeed, even Felix Mann, founder of the Medical Acupuncture Society and first president of the British Medical Acupuncture Society, has concluded: “the acupuncture points are no more real than the black spots that a drunkard sees in front of his eyes.”
The confusion is confounded by the fact that changes caused by stimulation of ‘acupuncture points’ are not unique to those points. Many clinical studies of acupuncture have used sham controls, that is, control needling has been applied at ‘sham’ points adjacent to or distant from ‘real’ acupuncture points. In general, when effects of acupuncture are evident, sham acupuncture appears to be almost as active as ‘real’ acupuncture. Needle sensation is not unique to acupuncture points and identical, transient, quick reflex responses of the sympathetic nervous system have been seen whether real or sham points are needled. Functional MRI studies have not demonstrated that stimulation of points thought to be specific to individual areas of the body (eg the eye) invoke changes in those specific regions of the brain. However, such studies do appear to have demonstrated that when one sticks a needle into the body, the body notices.
The mechanism(s) of action proposed for acupuncture are not unique to it. Rather, the results claimed for acupuncture are potentially easily explained by well-known mechanisms, including the placebo effect, a diffuse noxious stimulus (if one place hurts, another might not hurt as much), or an overestimation of effects due to the owner’s desire to please the therapist (a well-known psychological phenomenon).
Although a precise definition is elusive, placebos have been defined as “an epithet given to any medicine adopted to please rather than to benefit the patient”. Its existence only requires that any perceived improvement ‘follow’ a placebo intervention; there is no necessary causal link. If one were trying to invent a placebo, one could hardly do better than acupuncture. It’s wrapped in the mysteries of the Orient, it’s invasive, it involves human contact, it is a mildly painful stimulus, and it offers explanations (albeit often simplistic and unproven) for complex health problems that may easily sway lay people.
There is a proposed link between the purported pain-reducing effects of placebos and the internal secretion of opioids, although the association between placebo interventions and the role of various neuropeptides is far from understood. The situation is made even more confusing in light of the fact that endogenous opioid release is postulated as a mechanism of action for acupuncture. Accordingly, it may be that acupuncture and placebo effects are inseparable. And, in fact, current large trials in Germany seem to indicate that acupuncture reduces pain in the same amount of patients as does a credible placebo. Still, it is no surprise that therapies that affect the mental state can stimulate the secretion of endogenous opioids and other mediators. And the fact remains that known methods of increasing endogenous opioids, for example, exercise, which is inarguably beneficial for health, are generally not the primary method of treating disease, nor are special therapeutic claims made for such methods.
There is also, of course, the pain element, referred to as ‘diffuse noxious stimulus’. If you have a headache, have someone kick you in the shin; your head might not feel so bad afterwards. A noxious stimulus at one site interferes with the perception of pain at another site. In that regard, while one study found that acupuncture suppressed the pain response to a cutaneous prick or electrical stimulation of a rat’s tail, the most effective suppression was obtained by a simple pinch.
Then there is the expectation of treatment. Perceptions and expectations of treatment significantly affect determinations of treatment efficacy. For example, the style and gender of the acupuncturist, as well as the length of time of needling, all affect perceptions of treatment efficacy. Such nonspecific factors are inherent in acupuncture, couched, as it is, in terms of holism and Chinese mystery.
So what of acupuncture? Clearly, it has failed to demonstrate that it’s an important addition to health care, both over time and in the recent decades of scientific investigation.
After decades of investigation, acupuncture appears to be little more than an impressively contrived placebo. There seems to be little reason for people to waste time and money on this elaborate ritual (for themselves, or their horses).